Background, Genetic and Infectious screening
The most important part of the infertility work-up is obtaining screening history and blood work so we can evaluate any potential problems before you get pregnant. This blood test is designed to assess your general health and tests also for infectious problems that may interfere with a healthy pregnancy.
 Screening blood tests include: complete blood count including differential, blood group and type and Rh. Blood tests also screen for HIV antibodies, Hepatitis B and C surface antigens, immunity against Rubella and German measles, syphilis serology, and Chlamydia antibody, as well as hormonal testing for Thyroid Stimulating Hormone (TSH) and prolactin (PRL). A PAP smear should have been done within the last year. Approximately 30 ml (2 tablespoons) of blood will be taken from your arm while you lie down. It is best to have this blood test drawn after fasting since midnight because your cholesterol and triglyceride levels will be checked. Therefore, you should not eat breakfast on the day of your blood test.
Screening blood tests include: complete blood count including differential, blood group and type and Rh. Blood tests also screen for HIV antibodies, Hepatitis B and C surface antigens, immunity against Rubella and German measles, syphilis serology, and Chlamydia antibody, as well as hormonal testing for Thyroid Stimulating Hormone (TSH) and prolactin (PRL). A PAP smear should have been done within the last year. Approximately 30 ml (2 tablespoons) of blood will be taken from your arm while you lie down. It is best to have this blood test drawn after fasting since midnight because your cholesterol and triglyceride levels will be checked. Therefore, you should not eat breakfast on the day of your blood test.
We may order appropriate genetic screening based on your background and family history. Examples of genetic screening tests include evaluations for sickle cell anemia and/or cystic fibrosis.
Ovarian function/ovulation screening
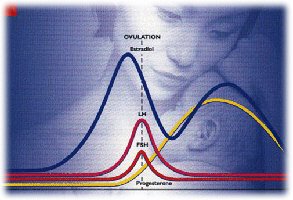 Disorders in the ovary account for about 30% of female related infertility. Our main questions are: 1. Are you ovulating? 2. How well do you ovulate (or what is the quality of eggs you produce)? Many women have premenstrual symptoms (bloating, breast tenderness) a few days before their menses. This is a good sign that you ovulate. Some women may have regular bleeding, but not actually ovulate. We may evaluate this question by ordering levels of Follicle Stimulating Hormone (FSH), or Luteinizing Hormone (LH),which are made by the brain (pituitary gland) in order to stimulate egg development in the ovary. We also may order a progesterone level, a hormone made by the ovary only after ovulation, or have you check your urine with an ovulation predictor kit (LH surge kit), which you can buy in the drug store.
Disorders in the ovary account for about 30% of female related infertility. Our main questions are: 1. Are you ovulating? 2. How well do you ovulate (or what is the quality of eggs you produce)? Many women have premenstrual symptoms (bloating, breast tenderness) a few days before their menses. This is a good sign that you ovulate. Some women may have regular bleeding, but not actually ovulate. We may evaluate this question by ordering levels of Follicle Stimulating Hormone (FSH), or Luteinizing Hormone (LH),which are made by the brain (pituitary gland) in order to stimulate egg development in the ovary. We also may order a progesterone level, a hormone made by the ovary only after ovulation, or have you check your urine with an ovulation predictor kit (LH surge kit), which you can buy in the drug store.
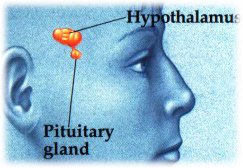 While the question of whether you ovulate is an important one, it is equally important toknow how well you ovulate. Some women may have regular, monthly, ovulatory periods, but the “quality” of their eggs may be reduced. This happens naturally as women age. By testing the FSH on the third day of the cycle, we can predict how well the ovary is making the eggs. These tests of “ovarian reserve” allows us to better predict how well your ovaries will respond to stimulation with fertility drugs, and help us to predict your potential pregnancy rate with infertility treatment.
While the question of whether you ovulate is an important one, it is equally important toknow how well you ovulate. Some women may have regular, monthly, ovulatory periods, but the “quality” of their eggs may be reduced. This happens naturally as women age. By testing the FSH on the third day of the cycle, we can predict how well the ovary is making the eggs. These tests of “ovarian reserve” allows us to better predict how well your ovaries will respond to stimulation with fertility drugs, and help us to predict your potential pregnancy rate with infertility treatment.
 This test, a day 3 FSH, is drawn on day 3 of your cycle, and is required by all women undergoing advanced infertility treatment. We will inform you if you are a candidate for testing. Sometimes we may need to stimulate the ovary a little to get even more information about how well the eggs are doing. In this case, we perform a clomiphene citrate challenge test (CCCT),where we draw an FSH on day 3 and day 10 of your cycle after you have taken 100 mg of clomiphene on day 5-9 of your cycle. We perform this test in all women over the age of 35, and in women with unexplained infertility. We can perform an intrauterine insemination (IUI) during the same cycle as your CCCT, potentially turning a diagnostic test into a therapeutic one.
This test, a day 3 FSH, is drawn on day 3 of your cycle, and is required by all women undergoing advanced infertility treatment. We will inform you if you are a candidate for testing. Sometimes we may need to stimulate the ovary a little to get even more information about how well the eggs are doing. In this case, we perform a clomiphene citrate challenge test (CCCT),where we draw an FSH on day 3 and day 10 of your cycle after you have taken 100 mg of clomiphene on day 5-9 of your cycle. We perform this test in all women over the age of 35, and in women with unexplained infertility. We can perform an intrauterine insemination (IUI) during the same cycle as your CCCT, potentially turning a diagnostic test into a therapeutic one.
Uterine evaluation
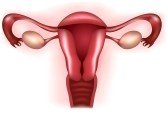 The uterus, or womb, is lined on the inside by a layer called the endometrium. This is where the developing pregnancy will implant. It is important to evaluate the uterine cavity, looking for potential problems such as uterine scar tissue,polyps, fibroids, or other structural defects in the uterus. These problems may interfere with a developing pregnancy, leading to miscarriage and/or infertility. The uterine evaluation will consist either of an X-ray study of the uterine cavity, a hysterosalpingogram (HSG) or a sonohysterogram, a special ultrasound test. If there are abnormalities on these tests, we may perform a hysteroscopy, a surgical procedure used to correct problems inside the uterus.
The uterus, or womb, is lined on the inside by a layer called the endometrium. This is where the developing pregnancy will implant. It is important to evaluate the uterine cavity, looking for potential problems such as uterine scar tissue,polyps, fibroids, or other structural defects in the uterus. These problems may interfere with a developing pregnancy, leading to miscarriage and/or infertility. The uterine evaluation will consist either of an X-ray study of the uterine cavity, a hysterosalpingogram (HSG) or a sonohysterogram, a special ultrasound test. If there are abnormalities on these tests, we may perform a hysteroscopy, a surgical procedure used to correct problems inside the uterus.
Tubal evaluation
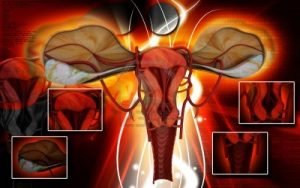 Problems with the fallopian tubes, such as tubal blockage, account for about 30% of female infertility problems. This is especially true in women who may have had a pelvic infection in the past. Blocked tubes and scar tissue can also be caused by abdominal infections such as appendicitis, prior surgeries, or endometriosis. We screen for problems on the fallopian tubes by performing a hysterosalpingogram (HSG). This test evaluates problems in both the uterus and the fallopian tubes (see above). If we find tubal blockage, we may perform a laparoscopy, a surgical procedure done to better diagnose and potentially correct tubal problems.
Problems with the fallopian tubes, such as tubal blockage, account for about 30% of female infertility problems. This is especially true in women who may have had a pelvic infection in the past. Blocked tubes and scar tissue can also be caused by abdominal infections such as appendicitis, prior surgeries, or endometriosis. We screen for problems on the fallopian tubes by performing a hysterosalpingogram (HSG). This test evaluates problems in both the uterus and the fallopian tubes (see above). If we find tubal blockage, we may perform a laparoscopy, a surgical procedure done to better diagnose and potentially correct tubal problems.
Endometrial biopsy
An endometrial biopsy, or biopsy of the lining of the uterus, may be done to look for a potential problem in the development of the endometrium called luteal phase defect. It may also be done to look for infectious problems.
